What is COVID Oximetry@home (CO@h)?
We have learnt a lot about how the COVID-19 virus can affect people differently.
For most people, the symptoms they experience are mild, but for a few individuals they are not unwell enough for immediate hospital care but can be at risk of silent hypoxia. Hypoxia occurs when levels of oxygen in the blood are lower than normal. If blood oxygen levels are too low, your body may not work properly. Blood carries oxygen to the cells throughout your body to keep them healthy. In silent hypoxia the oxygen level in the blood reduces but the individual experiences no worsening of symptoms such as respiratory distress/increased breathlessness.
It is important that care staff are able to detect early signs of such deterioration so the individual can be referred for appropriate treatment quickly.
Monitoring blood oxygen levels is achieved through the use of an oximeter, which measures the individuals pulse rate and the oxygen saturation rate in the blood.
For the individual and anyone supporting them on a day to day basis, this will indicate when/how to raise concerns of changes in their condition and symptoms and better support those at risk of deterioration through early identification.
Who can access CO@h from my Care Home?
CO@h is a service suitable for adults more likely to experience worsening or life-threatening silent hypoxia. Criteria are:
- Diagnosed with COVID: either clinically or via a positive test result and
- Symptomatic
and either
- Aged 65 years or older or
- Under 65 years and clinically vulnerable to COVID.
Some individuals may not wish to be monitored and may decline the regular monitoring through pulse oximetry, for example if their TEP form states they do not want to go to hospital. If a patient declines to be monitored, it is important to ensure that the risks associated with not monitoring their oxygen level have been explained and a note recorded in their care record.
How do I enrol a resident in this service?
If you identify a resident who qualifies for CO@h, please contact your named clinical lead or the resident’s registered GP. They will need to assess the patient as being suitable for the CO@h service, and ensure they are not so unwell that they should be treated in hospital.
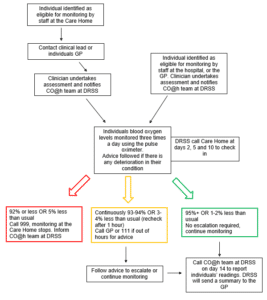
What happens next?
The patient will be assessed by a Primary Care clinician, to see if they are suitable for the service, and well enough to remain in the Care Home whilst being monitored. If they are seen face to face, this will involve a baseline reading of their oxygen saturations, but this assessment may be done remotely. If so, you will be asked to take the patients reading using one of the oximeters provided to your care home. The GP will send an alert to our CO@h team at Devon Referral Support service (DRSS) who are centrally coordinating the service.
After you have taken the baseline oximeter reading, you should record it on the log sheet at the back of this pack and make a note in the residents’ care plan that they need to have further oximeter readings taken and recorded three times per day.
You should then continue to take and record the residents reading three times a day, every day, until it has been 14 days since the onset of their symptoms. The CO@h team will call the care home on days 2, 5 and 10 of the resident being monitored to centrally store their readings.
All being well, on day 14, you should call the central CO@h team at DRSS on 01626 204950 (Monday-Sunday, 9.00am-5.00pm) to provide the final readings from their time being monitored. The CO@h team at DRSS will record these and provide a summary to the GP.
If their oxygen saturations deteriorate at any time during this period, please follow the advice below.
You should call 999 immediately if they experience the following:
- Blood oxygen levels that are 92% or less or have fallen by 5% or more from their usual level
- They are unable to complete short sentences when at rest due to breathlessness
- Their breathing gets worse suddenly.
Or If they develop these more general signs of serious illness, for example:
- They cough up blood
- They feel cold and sweaty with pale or blotchy skin
- Develop a rash that does not fade when you roll a glass over it
- Collapse or faint
- Become agitated, confused or very drowsy
- Stop passing urine or are passing much less than usual.
You should tell the operator they are under monitoring via the CO@H service from their care home. A minority of people with COVID-19 will experience these more severe symptoms. These require urgent medical attention.
Ring their GP Practice or NHS 111 as soon as possible if they experience any new or an increase in any the following COVID-19 symptoms:
• Feeling breathless or difficulty breathing, especially when standing up or moving
• Severe muscle aches or tiredness
• Shakes or shivers
• If their blood oxygen levels are 94%, 93% or are 3-4% lower than their usual reading after a re-test one hour later
• Sense that something is wrong (general weakness, severe tiredness, loss of appetite, peeing much less than normal – unable to perform simple tasks which they would ordinarily be able to).
You should tell the operator they are under monitoring via the CO@H service from their Care Home.
If the patient deteriorates and goes to hospital, they will end their monitoring. You should call the CO@h team at DRSS to let them know this, and to provide the readings to date.
On discharge, the secondary care team may wish the resident to be monitored again if they are still experiencing COVID symptoms and are within 14 days of symptom onset. If so, they will assess them and refer them to the CO@h team who will notify you.
Frequently asked questions
Q: How long will the patient be monitored by a member of staff?
A: Normally for 14 days after the onset of the symptoms. However, if they go to hospital during this time, they will stop being monitored by you, although they may be referred again when they leave hospital.
Q: What happens if the resident has already finished their 14 days but I am still worried about them having symptoms of coronavirus?
A: Depending on the symptoms you should call their GP (or 111 if out of hours) or if they are deteriorating rapidly, please contact 999.
Q: What about residents under the age of 16 years?
A: As the effects of COVID-19 can affect people under the age of 16 years differently, the CO@h service is not suitable to deliver appropriate monitoring for this patient group. If you are concerned about any of your patients under the age of 16 years, please contact their GP, or call 999 if you are seriously concerned.
Q: What if there are issues with the oximeter whilst I am monitoring a resident?
A: The CO@h team at DRSS can organise for another one to be loaned for your use. Please call them on 01626 204950 if this happens.
Useful links
National Deterioration forum, CO@h page
Translated patient information leaflet with patient diary and videos on use of oximeter
RCGP paper on Virtual Wards, Silent Hypoxia and improving COVID outcomes
COVID Oximetry at Home – Quick Reference Guide
Pulse oximetry monitoring for patients who have COVID19 (or suspected), symptomatic, and either over 65 or Clinically Extremely Vulnerable.
COVID Oximetry at Home – Monitoring log sheet
Please print or store as many of these pages as needed for multiple individuals.